In it for the Long Haul
The internationally recognised Heinz Nixdorf Recall Study has been investigating cardiovascular diseases for more than 23 years. There’s no end in sight, and that’s a good thing.
By Ulrike Bohnsack
The wealthy suffered from calcification of arteries and its con-sequences even in antiquity. Today, cardiovascular diseases stand for a depressing record worldwide: they are the most common cause of death, first and foremost heart attacks, strokes, and coronary heart disease. What clogs the vessels, what keeps them healthy, and how is it possible to determine one’s individual risk? Researchers have been occupied with these questions for a long time, but in the late 1990s a team at Essen University Hospital attempted a new approach: Instead of focusing on patients as previously, they decided to study a broad cross-section of the population – including healthy people – over a long-term period. Accordingly, they randomly selected just under 5,000 men and women between the ages of 45 and 75 in the Ruhr metropolitan area and began in 2000 to give them regular check-ups and detailed surveys.
It was the first study of its kind in Europe and has been followed closely worldwide – and for good reason: it is representative of a conurbation in an industrial country, has been running for 23 years without interruption, and produces valuable data and findings again and again, particularly since around 3,000 grown children and life partners of the first cohort have been participating since 2013 as well. ‘It is thus becoming ever clearer which factors interact in these widespread diseases,’ says Prof. Dr Börge Schmidt. ‘And as we know today, there are a lot of them: heredity, other diseases, psychosocial aspects, lifestyle, and environmental influences.’
Schmidt himself has been collaborating on the study since the second phase. He was initially involved interviewing study participants as a biology student starting in 2006. Then his tasks and responsibility grew. Today he serves as professor of epidemiology and deputy director of the Institute for Medical Informatics, Biometry, and Epidemiology (IMIBE). He conducts the large-scale population studies and conducts research in international collaboration. When the 46-year-old talks about his work, every sentence exudes enthusiasm, also about the participants, ‘who really want to take part and have done so for decades in some cases.’
SIGNIFICANCE IMPROVES CONSTANTLY
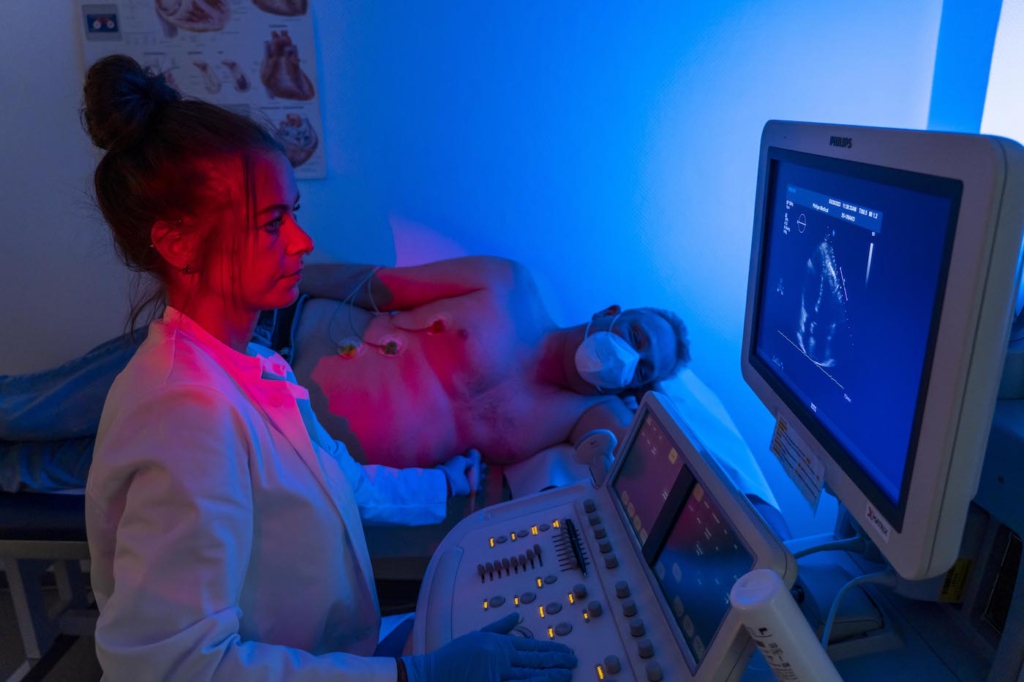
The subjects are examined with modern imaging methods, such as ultrasound and CT scanning. In addition, an ECG is made, genetic material analysed, blood, urine, body mass index, and respiration measured, cognitive abilities tested – that is, thinking and perception –, psychosocial stressors, and life circumstances surveyed. These comprehensive examinations are conducted about every five years. In contrast, participants complete the extensive questionnaire annually.
Over the years, it becomes clear who falls ill, when, and why. As the surveys cover several generations, their significance for explaining the causes of diseases improves constantly, emphasises IMIBE director Prof. Dr Andreas Stang: ‘Assumptions from other studies are confirmed, and new knowledge is acquired.’
Thus, the Heinz Nixdorf Recall Study made it clear for the first time for the general population in Europe how strong the connection is between calcification of the coronary vessels and risk of heart attack. ‘The common practice today for predicting cardiovascular diseases is to detect coronary calcification with imaging methods, and the Essen study played an instrumental role in this development,’ says Stang. However – and this is another finding –, it does not make sense to send patients back to get a CT every few years to receive a more precise prognosis. ‘A single measurement of calcification is usually sufficient to be able to make a good assessment of a person’s risk.’
POVERTY AS A RISK FACTOR
People who live in the city are at greater risk of suffering from certain diseases, even more so if they live close to a busy street. This is due to noise and fine particulate air pollution, the study shows. Rents are cheaper on major roads, which is why they usually attract poorer families. The researchers were able to determine that social inequality affects health. ‘For example, we took a look at the biomarker cystatin,’ says Schmidt. ‘This laboratory value for kidney function also provides evidence of cardiovascular risks and was distributed unevenly among our subjects as well: people with a low income and a lower level of education had lower values.’
How much of a difference do genes make? That’s a question the research team is currently addressing. ‘There is definitely a hereditary component, but it doesn’t explain everything,’ the scientist stresses. ‘Our hypothesis is that parents pass on not only a negative predisposition to coronary calcification to their children but also unfavourable behaviours. If I grow up as a child in a family in which a lot of meat, sugar, and soft drinks are on the menu, that will presumably also influence my diet as an adult.’ An unfavourable risk profile is thus perpetuated in the family, laying the foundation for diabetes, overweight, heart problems, and even dementia.
‘Nevertheless, poor genes need not automatically lead to poor health. Environmental and social factors play a role as well.’ Schmidt provides an example: ‘There’s a gene that has a strong influence on dementia, Alzheimer’s disease, or their early stages in the form of mild cognitive impairment. In our studies, we found that people with a poor genotype and a high level of education do not have a higher risk of early cognitive deficits at all. A poor genotype and a low level of education, on the other hand, were highly unfavourable. That was not previously clear.’
New questions – and new insights – are constantly emerging for the research team, about everything from depressions and migraines to chronic renal insufficiency and, currently, symptoms of long COVID. ‘We’re putting all our energy into ensuring that the Heinz Nixdorf Recall Study continues to receive funding over the next decades. Ideally,’ says Börge Schmidt, ‘we want it to run until the very last participant is deceased.’
HEINZ NIXDORF RECALL STUDY
How can the prediction of cardiovascular diseases be improved? That’s the main question of the population-based cohort study in the Ruhr area, which was launched in 2000 and encompasses just under 8,000 participants, including 1,878 families. Using their health data, scientists are conducting epidemiological studies to determine how common diseases are in the population, whether they are hereditary, and how they are affected by lifestyle, social, and environmental influences.
The studies are being funded by the Heinz Nixdorf Foundation. They are headed by the professors Andreas Stang, Börge Schmidt, and Raimund Erbel from the Institute for Medical Informatics, Biometry, and Epidemiology (IMIBE).
Main image: Regular blood work is done on the participants. | © Jochen Tack



